MobileODT Received 2.3 Million Dollars From the US National Cancer Institute
27 January, 2021
The Tel Aviv based company developed a device that will allow cervical cancer screening using a smartphone. The grant will fund a pilot with 10,000 female participants
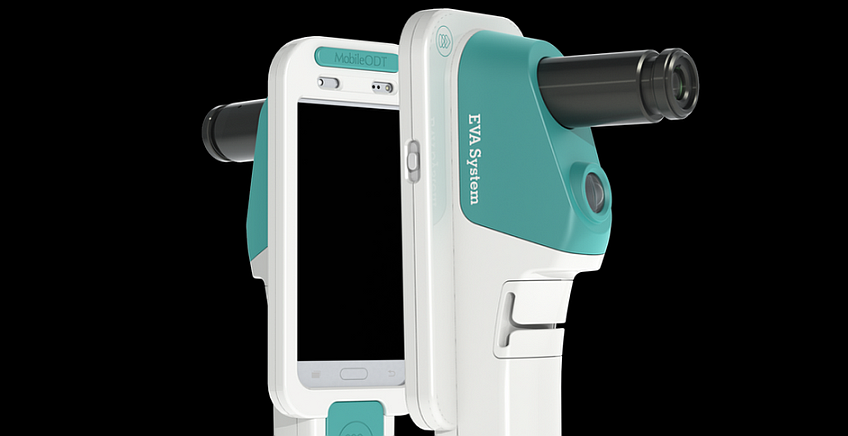
MobileODT, a Tel Aviv based company, that developed a device that allows cervical cancer screening using a smartphone, was rewarded with a grant of 2.3 million dollars from the United States National Cancer Institute (NCI). The grant is awarded to companies that have developed innovative technologies or treatments that help the fight against cancer. The grant will be used by MobileODT to fund a widespread pilot in the US that will test the efficacy of the company’s solution as an alternative diagnostic tool to the accepted screening methods, including the vaginal colposcopy, which requires imaging equipment. The experiment will commence in the third quarterer of 2021 and about 10,000 women will participate. The experiment will be performed in collaboration with the BHI organization, which promotes research and development in the cervical cancer field, and with the assistance of the Cleveland Clinic.
According to the World Health Organization’s (WHO) assessment, about 275 thousand women die from cervical cancer every year, mostly because of lack of early detection of the disease. The acceptable method today for early detection of cervical cancer is the PAP test, in which a cell sample is collected from the cervix and examined by microscope. If irregularities are discovered, the woman must undergo a colposcopy test, which creates imaging of the cervix. Despite this, according to WHO data, about 85% of women in the world do not have proper access to these tests.
A Mobile Colposcopy Using Smartphones
MobileODT, which was established in 2012 and is now run by the CEO Leon Boston, developed an inexpensive and mobile kit called EVA System, which is based on the smartphone’s photography and processing abilities and allows it to perform the vaginal colposcopy. The kit includes a zoom lense that is attached to the smartphone camera and a powerful lighting unit that allows clear imaging of the cervix. After the test, the images can be sent to gynecologists and experts through the application for diagnosis. In addition, the product also includes a smart decoding of the test, based on algorithms developed using machine learning performed on large databases of patient’s cervical imaging.
This assessment allows nurses, midwives and therapists to simply perform the diagnostic test even in remote locations and countries in which medical infrastructure is lacking, and thus help lessen the cervical cancer mortality rates. The EVA System kit which received FDA approval in 2016, is sold today in about 30 countries and is in use in 60 clinics in the US.
The Situation in Israel
This week was the international cervical cancer awareness week and Israel Cancer Association (ICA) together with the Ministry of Health published the morbidity data among women in Israel. In 2017, 248 women were diagnosed with invasive cervical cancer and 717 women with stage 3 cervical intraepithelial neoplasia. On the international scale, compared to the OECD countries, Israel is rated relatively low on the scale (33rd out of 36). The ICA explains that cervical cancer is preventable in most cases by receiving the Human Papillomavirus (HPV) Vaccine at a young age, and early detection by screening.
Dr. Mario Beiner, the head of the Gynecologic Oncology unit at Meir Medical Center, and president of the Israeli Association of Gynecologic Oncology (ISGO): “Over the past few years, we have seen an improvement in the number of women coming in for PAP tests. The rate of women who have undergone PAP tests as a screening method has grown from 48.1% to 51.5% and the rate of women who haven’t had a PAP test in the last 5 years has gone down from 39% to 34.8%. Nevertheless, unfortunately, the screening rate is still low, especially in the weaker socio-economic populations. In addition, the HPV vaccination rate, given for free to children in school, is still low and stands at less than 60%. From my experience with patients, they don’t get the information from their family doctors and gynecologists that even if they were not vaccinated while at school, it is still advisable to get the vaccine through their HMOs up to the age of 45.”